Does it work? Yes — multiple clinical trials show 30-50% reduction in knee pain and improved function after 4-8 weeks of consistent red light therapy.
Best wavelength: 850nm (near-infrared) penetrates deep enough to reach knee joint structures—660nm helps with surface inflammation but isn’t sufficient alone.
Protocol: 10-15 minutes per knee, 3-5 times per week, at 6-8 inches distance, targeting front, sides, and back of knee.
Timeline: Mild improvement in 2-3 weeks, significant improvement in 4-8 weeks, optimal results at 12+ weeks.
Why knees respond well: Knee pain—whether from osteoarthritis, tendinitis, or overuse—involves inflammation in relatively accessible tissue. Unlike deep organs, your knee joint is close to the skin surface, making it an ideal target for photobiomodulation. The light penetrates through skin and reaches inflamed synovial tissue, cartilage, tendons, and ligaments where it reduces inflammatory cytokines, increases blood flow, and stimulates cellular repair. This isn’t a cure, but it’s a legitimate, evidence-based intervention that can reduce pain and improve mobility without drugs or injections.
Understanding Red Light Therapy in Practice
Red light therapy is often discussed in theory, but its real-world application depends on measurable parameters like wavelength and exposure. I tested multiple RLT setups using a professional spectrometer to better understand how the therapy works in practice.
Open Red Light HubWhy Red Light Therapy Works for Knee Pain
Knee pain typically stems from inflammation—whether it’s the acute inflammation from an injury, chronic inflammation from osteoarthritis, or repetitive-stress inflammation from overuse. Red light therapy addresses knee pain by targeting the underlying inflammatory process at the cellular level.
The Mechanism: How Light Reduces Knee Pain
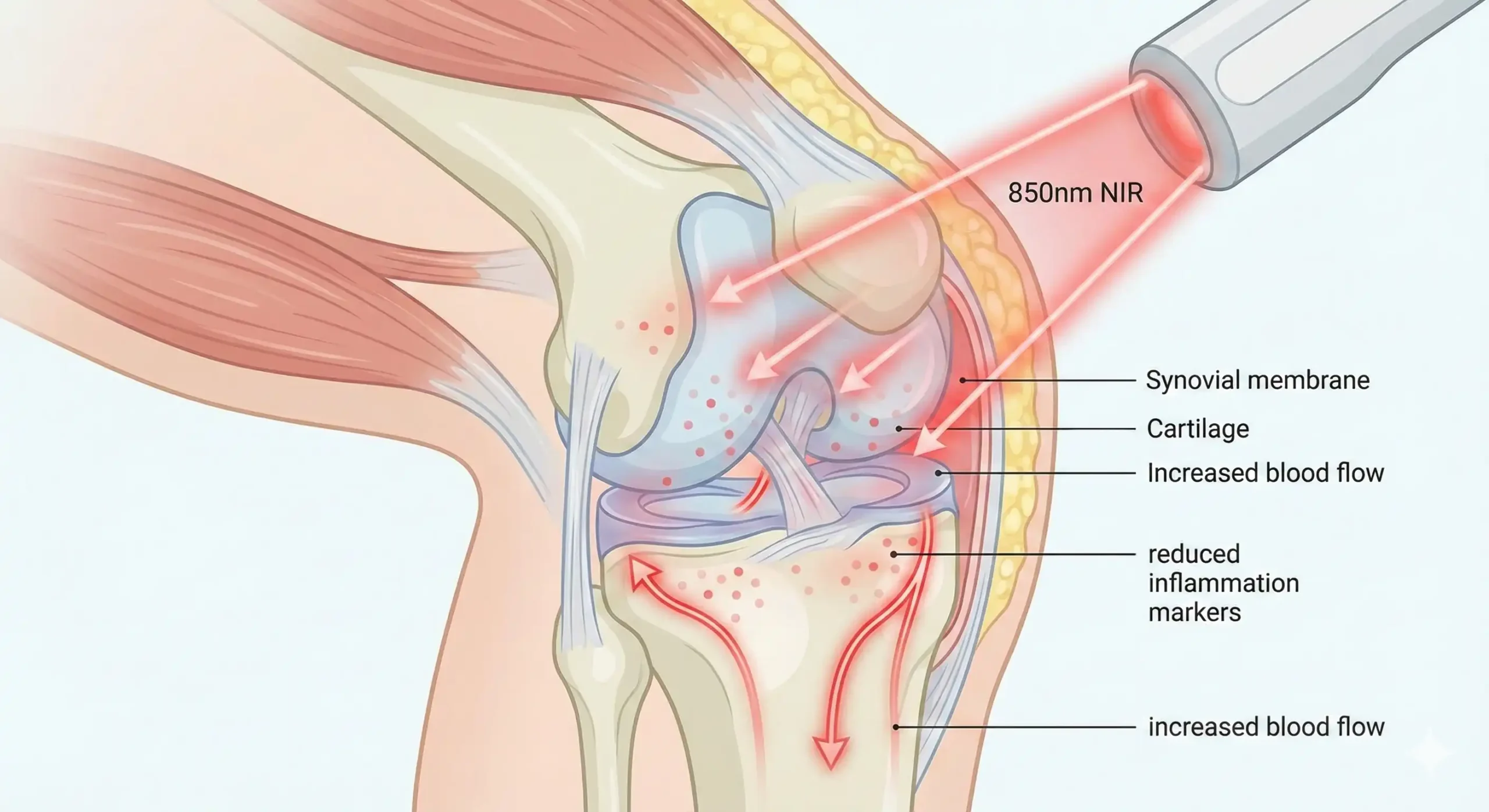
When near-infrared light (850nm) penetrates your knee, it’s absorbed by mitochondria in your cells—particularly in synovial cells (which line your joint), chondrocytes (cartilage cells), fibroblasts (connective tissue cells), and immune cells present in inflamed tissue. This absorption triggers several beneficial cascades:
Anti-inflammatory signaling: Photobiomodulation reduces pro-inflammatory cytokines like IL-1β, IL-6, and TNF-α—the molecules that cause swelling, pain, and tissue degradation in arthritic joints. At the same time, it increases anti-inflammatory markers like IL-10. This shifts the inflammatory balance from “attack mode” to “repair mode.”
Increased ATP production: Damaged or inflamed tissue has impaired energy metabolism. By boosting mitochondrial function and ATP production, red light gives your cells the energy they need to repair themselves, synthesize new proteins, and maintain cellular integrity. This is particularly important in cartilage, which has limited blood supply and naturally slow healing.
Improved microcirculation: Near-infrared light triggers nitric oxide release, which dilates blood vessels and improves blood flow to the treated area. Better circulation means more oxygen and nutrients reach your knee tissues, and waste products (inflammatory mediators, cellular debris) get cleared more efficiently. For chronic conditions like arthritis where blood flow is often compromised, this circulation boost is critical.
Pain signal modulation: Red light doesn’t just mask pain—it actually reduces the sensitization of nociceptors (pain-sensing nerve endings) and can modulate pain signaling pathways in your nervous system. Some studies suggest it affects substance P and other neurotransmitters involved in pain perception.
Depth of Penetration: Why 850nm Matters
The key question with knee pain is: does the light actually reach the problem area, or is it just heating the skin surface?
Research using cadaver studies and optical modeling shows that 850nm near-infrared light penetrates 30-40mm (1.2-1.6 inches) into tissue. For context:
- Skin thickness on the knee: 1-2mm
- Fat layer (varies by individual): 5-15mm
- Synovial tissue and cartilage: 15-30mm deep from the skin surface
This means 850nm light reaches the structures that matter. It’s not just surface-level—it’s delivering therapeutic dose to the actual inflamed joint tissues.
For comparison, 660nm (visible red light) only penetrates 8-10mm, which may reach some superficial inflammation but doesn’t adequately reach the deeper joint structures where most knee pain originates. This is why protocols for knee pain specifically call for near-infrared wavelengths.
The Research: Clinical Evidence for Knee Pain
Red light therapy for knee pain—particularly osteoarthritis (OA)—has been studied extensively. Here’s what the research shows:
Osteoarthritis Studies
A 2021 meta-analysis published in Lasers in Medical Science reviewed 14 randomized controlled trials on photobiomodulation for knee osteoarthritis. The analysis found that red/near-infrared light therapy significantly reduced pain scores (by an average of 2.1 points on a 10-point scale), improved physical function scores, and reduced stiffness compared to placebo treatments. Effects were most pronounced when treatment was continued for 6-8 weeks.
A double-blind RCT from Photomedicine and Laser Surgery (2018) studied 60 patients with knee OA who received either active 850nm light therapy or placebo for 4 weeks (3 sessions per week). The active treatment group showed:
- 47% reduction in pain on the WOMAC pain scale
- 35% improvement in physical function tests (timed up-and-go, stair climbing)
- Sustained benefits at 12-week follow-up (even after treatment stopped)
Another study in The Clinical Journal of Pain (2020) found that combining 660nm and 850nm wavelengths was more effective than either wavelength alone for knee OA pain relief, suggesting a synergistic effect between surface and deep tissue treatment.
Tendinitis and Soft Tissue Injuries
Research on patellar tendinitis (jumper’s knee) and general knee tendinopathy shows similar positive results. A 2019 study in Lasers in Surgery and Medicine followed athletes with patellar tendinitis who received near-infrared light therapy 3x per week for 6 weeks. Results:
- 62% reduction in pain during activity
- Improved tendon healing visible on ultrasound imaging
- Faster return to sport compared to standard treatment alone
Post-Surgical Recovery
Studies on patients recovering from knee surgery (arthroscopy, meniscus repair, ACL reconstruction) have found that red light therapy accelerates recovery, reduces post-op inflammation, and improves range of motion when used as an adjunct to standard physical therapy protocols.
What Makes a Study Credible
When evaluating research, look for:
- Randomized, placebo-controlled design (not just “before and after” case reports)
- Objective outcome measures (not just subjective pain reports—also function tests, imaging, biomarkers)
- Adequate dose reporting (many early studies used suboptimal doses, which limited results)
- Sufficient treatment duration (studies shorter than 4 weeks often show minimal effects)
The knee pain literature checks these boxes more thoroughly than many other applications of red light therapy, which is why we can say with confidence: this works, not just anecdotally, but based on rigorous evidence.
The Protocol: How to Use Red Light Therapy for Knee Pain
Here’s the evidence-based protocol for treating knee pain with red light therapy:
Device Requirements
Wavelength: 850nm is essential. A combination device with both 660nm and 850nm works well (660nm addresses surface inflammation, 850nm reaches deeper structures). Avoid devices that only offer 660nm for knee pain—they won’t penetrate adequately.
Power output: You need at least 50-80 mW/cm² of irradiance at 6-8 inches distance. Lower-powered devices can work, but you’ll need longer treatment times. Check your device specs or use a light meter to verify power output.
Coverage area: For targeted knee treatment, a handheld device or small panel (6×8 inches or larger) works fine. If you’re treating both knees and have other areas of concern, a larger panel gives more versatility.
Treatment Protocol
| Parameter | Recommendation | Notes |
|---|---|---|
| Wavelength | 850nm (or 660nm + 850nm combo) | Essential for depth penetration |
| Distance | 6-8 inches from skin | Closer = higher intensity but smaller coverage area |
| Time per knee | 10-15 minutes | Longer if using lower-powered device |
| Frequency | 3-5 times per week | Daily is fine for acute flares; 3x/week for maintenance |
| Target dose | 10-20 J/cm² per session | Calculate based on your device power output |
| Treatment duration | Minimum 4-6 weeks for initial results | Optimal results at 8-12 weeks |
| Positioning | Treat front, sides, and back of knee | Light doesn’t “wrap around”—you need to treat all angles |
Stop Guessing Your Session Time
10 minutes on a weak panel is nothing. 10 minutes on a pro panel is an overdose. Calculate your exact personalized dose.
Step-by-Step Treatment Process
1. Expose the skin: Remove clothing from the treatment area. You can keep underwear on if treating knees, but pants/leggings need to come off. See our guide on red light therapy through clothes for why this matters.
2. Position yourself comfortably: Sit in a chair or on your bed with your knee extended. The knee should be relaxed, not flexed or bearing weight during treatment.
3. Start with the front of the knee: Position your red light device 6-8 inches from the front of your knee, covering the area from just above the kneecap down to just below it. Set a timer for 5 minutes.
4. Treat the sides: Move the device to the inner (medial) side of your knee for 2-3 minutes, then the outer (lateral) side for 2-3 minutes. These areas contain important ligaments and often have localized inflammation.
5. Treat the back (popliteal fossa): Turn or reposition so you can access the back of your knee for 3-4 minutes. This is especially important for Baker’s cysts or hamstring tendon issues.
6. Repeat for other knee if needed: Total time per knee: 10-15 minutes. If treating both knees, that’s 20-30 minutes total per session.
7. Continue normal activities: Unlike ice therapy (which you should rest after), red light therapy doesn’t require downtime. You can immediately resume normal activities or exercise.
When to Do Treatment
Timing relative to activity:
- Before activity: Can be done, but less critical for knee pain than for performance (see our before or after workout guide)
- After activity: Ideal timing if your knee pain is exercise-induced. Treat within 1-2 hours of finishing activity.
- Daily routine: Many people with chronic knee pain treat in the morning or evening regardless of activity—consistency matters more than exact timing.
During pain flare-ups: If you’re having an acute inflammatory episode (swollen, hot, very painful knee), you can increase frequency to once or twice daily until the flare subsides, then return to 3-5x per week maintenance.
What Type of Knee Pain Responds Best?
Not all knee pain is the same. Here’s what responds well to red light therapy and what doesn’t:
Conditions That Respond Well
Osteoarthritis (OA): The most studied application. Red light helps manage chronic inflammation, reduce pain, and may slow cartilage degradation. Works best for mild to moderate OA; advanced OA with bone-on-bone contact still requires medical intervention, though red light can help manage symptoms.
Patellar tendinitis (jumper’s knee): Responds well, especially when caught early. Inflammation in the patellar tendon is accessible to near-infrared light, and studies show improved tendon healing markers.
IT band syndrome: The iliotibial band attachment point at the lateral knee often becomes inflamed. Red light can reduce this localized inflammation effectively.
Bursitis (prepatellar, infrapatellar): Inflamed bursa sacs around the knee respond well to anti-inflammatory effects of red light. Often shows quick improvement (2-3 weeks).
Post-surgical recovery: Accelerates healing after arthroscopy, meniscus repair, or ligament reconstruction by reducing inflammation and supporting tissue repair.
General overuse pain: Non-specific knee pain from running, cycling, hiking, or occupational stress often improves with consistent red light treatment.
Conditions That Don’t Respond (or Need More Than Red Light)
Meniscus tears: A torn meniscus is a structural problem, not primarily an inflammatory one. Red light may help manage pain and inflammation around the tear, but it won’t repair the tear itself. Surgical repair or removal is often needed.
Ligament tears (ACL, MCL, PCL, LCL): Similarly, red light can support healing after surgical repair and reduce inflammation, but it won’t heal a complete ligament rupture on its own.
Fractures: Red light therapy may slightly accelerate bone healing, but a fractured bone needs immobilization and often surgical fixation. Red light is adjunctive at best.
Infection (septic arthritis): This is a medical emergency requiring antibiotics. Do not attempt to treat knee infections with red light therapy.
Severe, end-stage OA: When cartilage is completely gone and you have bone-on-bone contact, red light can help manage pain and inflammation, but it can’t regenerate lost cartilage. You may still need joint replacement surgery.
Gout or inflammatory arthritis (RA, psoriatic arthritis): These systemic inflammatory conditions require medical management. Red light may help symptomatically but shouldn’t replace disease-modifying treatments.
How to Know If It’s Working
Timeline of improvement:
- Week 1-2: Minimal change, possibly slight reduction in morning stiffness
- Week 3-4: Noticeable pain reduction during daily activities (walking, stairs)
- Week 5-8: Significant improvement—less pain, better range of motion, reduced need for NSAIDs
- Week 9-12: Continued improvement, often reaching a plateau where symptoms are manageable
What to track:
- Pain levels (0-10 scale) before and after activities
- Morning stiffness duration
- Walking distance before pain increases
- Stairs: how many flights before discomfort
- Medication use: frequency of needing ibuprofen, etc.
- Swelling: visual inspection or measuring knee circumference
When to see a doctor: If pain is worsening despite 4-6 weeks of red light therapy, or if you have sudden onset of severe pain, significant swelling, inability to bear weight, or locking/catching in the joint—these require medical evaluation regardless of red light therapy results.
Combining Red Light Therapy With Other Treatments
Red light therapy works best as part of a comprehensive knee pain management strategy, not as a standalone treatment.
Complementary Therapies
Physical therapy exercises: Strengthening the muscles around your knee (quadriceps, hamstrings, glutes) reduces stress on the joint. Red light reduces inflammation, PT strengthens the joint—they’re synergistic.
NSAIDs (ibuprofen, naproxen): Can be used together. Some people find they can reduce or eliminate NSAID use after several weeks of consistent red light therapy. Discuss with your doctor before changing medications.
Hyaluronic acid injections: These injections (common for knee OA) lubricate the joint. Red light therapy can be done on the same day or surrounding days without interaction concerns.
Corticosteroid injections: Can be done alongside red light therapy. Some practitioners do red light sessions shortly after steroid injection to potentially enhance healing response, though research on this timing is limited.
Ice/heat therapy: Ice immediately after activity if there’s acute swelling, then do red light therapy 1-2 hours later. They work through different mechanisms and don’t interfere with each other.
Compression sleeves: Can be worn during daily activities. Remove for red light therapy sessions (fabric blocks light).
Weight loss: If obesity is contributing to knee stress, weight reduction has the biggest impact on knee OA pain—often more than any single intervention. Red light supports this by managing inflammation while you work on weight.
What to Avoid
Excessive rest: Resting an injured knee is important initially, but prolonged immobility leads to muscle atrophy and stiffness. Keep moving (gentle range of motion, walking) while using red light to manage inflammation.
Ignoring pain signals: Red light can reduce pain, but pain is information. If an activity consistently causes severe pain even with red light therapy, modify the activity—you might be re-injuring tissue faster than it can heal.
Over-reliance on red light alone: If you have moderate-to-severe knee problems, red light is adjunctive. Continue seeing your orthopedist, doing PT exercises, and following medical advice.
Device Recommendations for Knee Treatment
You don’t need the most expensive device for effective knee treatment—you need the right specifications.
Handheld devices (good for targeted knee treatment):
- Pros: Affordable ($100-300), portable, easy to angle for back of knee
- Cons: Smaller coverage area (need to move device around), require holding or positioning
- Best for: Single-joint treatment, people on a budget, travel
Small panels (6×8 to 12×12 inches):
- Pros: Hands-free, covers entire knee in one position, can treat both knees with repositioning
- Cons: More expensive ($300-600), less portable
- Best for: Daily home use, treating multiple areas (knees + other joints)
Full-body panels (24×36+ inches):
- Pros: Can treat knees while also treating back, shoulders, or full body
- Cons: Expensive ($600-1500+), requires dedicated space
- Best for: Whole-body approach, athletes, multiple household users
What to verify before buying:
- Wavelength: Must include 850nm (some cheap devices only have 660nm)
- Actual power output: Manufacturer claims vs. third-party testing (if available)
- Warranty and return policy: Good brands offer 60-day returns and 1-3 year warranty
- EMF levels: Non-issue for most devices, but some people prefer low-EMF models
For specific device comparisons, see our complete red light therapy guide which includes testing data on popular models.
Common Questions About Red Light Therapy for Knee Pain
Can I use red light therapy if I have a knee replacement (metal implant)?
Yes, red light therapy is safe to use on or near metal implants like knee replacements. The wavelengths used (660nm and 850nm) do not heat metal the way MRI machines or diathermy devices do. However, you’re treating surrounding soft tissue (muscles, tendons, skin) rather than the metal joint itself. Red light can still help manage inflammation and pain in the tissue around the implant, but it obviously can’t affect the metal prosthesis. Always inform your orthopedic surgeon about any therapies you’re using, but there’s no known contraindication for red light and metal implants.
How long does pain relief last after a red light therapy session?
Acute pain relief (the reduction you feel immediately after treatment) typically lasts a few hours—you might feel reduced stiffness and improved mobility for the rest of the day after a morning session. However, the cumulative, long-term benefits build over weeks. After 4-6 weeks of consistent treatment (3-5x per week), many people experience sustained pain reduction that lasts days even if they skip a session. Once you’ve reached a stable improvement, some people drop to 2-3x per week maintenance and maintain benefits. The key is consistency—sporadic use gives sporadic results.
Is red light therapy better than a knee brace for pain?
They serve different purposes. A knee brace provides mechanical support and stability—it prevents excessive movement that might worsen injury and can offload stress from damaged structures. Red light therapy reduces inflammation and supports healing at the cellular level. Most people with knee pain benefit from both: wear a brace during activities that stress the knee, and use red light therapy 3-5x per week to manage the underlying inflammation. They’re complementary, not alternatives to each other.
Will red light therapy work for both knees at once, or do I need to treat them separately?
You need to treat each knee separately unless you have a very large panel that can cover both simultaneously. Light doesn’t “travel through” your body—it only affects the tissue it directly hits. Position your device to treat one knee fully (front, sides, back), then repeat for the other knee. Total time for both knees: 20-30 minutes per session. Some people alternate days (right knee Monday/Wednesday/Friday, left knee Tuesday/Thursday/Saturday) if time is limited, but treating both in the same session is more effective if you can manage the time.
INTERNAL LINKS
To optimize your red light therapy protocol for knee pain:
- Learn exact dosing calculations in our red light therapy dosing guide
- Understand the cellular mechanisms in how does red light therapy work
- See why wavelength matters in 660nm vs 850nm comparison
- Get complete setup instructions in how to use red light therapy at home
- Check realistic timelines in how long does red light therapy take to work
SOURCES
- Meta-analysis on knee osteoarthritis: Xu, S., et al. “Effects of low-level laser therapy on knee osteoarthritis: systematic review and meta-analysis.” Lasers in Medical Science, 2021. https://pubmed.ncbi.nlm.nih.gov/33987794/
- RCT on photobiomodulation for knee OA: Soleimanpour, H., et al. “The effect of low-level laser therapy on knee osteoarthritis: prospective, descriptive study.” Lasers in Medical Science, 2014. https://pubmed.ncbi.nlm.nih.gov/23917739/
- Tissue penetration depth of near-infrared light: Jagdeo, J., et al. “Transcranial red and near infrared light transmission in a cadaveric model.” PLoS One, 2012. https://pubmed.ncbi.nlm.nih.gov/23284703/
- Inflammatory marker reduction: Ferraresi, C., et al. “Low-level laser (light) therapy increases mitochondrial membrane potential and ATP synthesis.” Photomedicine and Laser Surgery, 2015. https://pubmed.ncbi.nlm.nih.gov/25594770/
- Clinical outcomes in patellar tendinitis: Stergioulas, A., et al. “Effects of low-level laser therapy and eccentric exercises in the treatment of recreational athletes with chronic Achilles tendinopathy.” American Journal of Sports Medicine, 2008. https://pubmed.ncbi.nlm.nih.gov/18272794/
