Does it work? Yes—red light reduces acne inflammation by 30-50% in 4-8 weeks, but doesn’t kill bacteria like blue light does.
Best wavelength: 660nm (red) for inflammation reduction + 415nm (blue) for bacteria killing = best combination.
Protocol: 10-15 minutes per day, 5-6 inches from face, 5-7 days per week for 4-8 weeks minimum.
Realistic expectations: Reduces inflammatory acne (papules, pustules) significantly; less effective for cystic acne or comedones (blackheads/whiteheads).
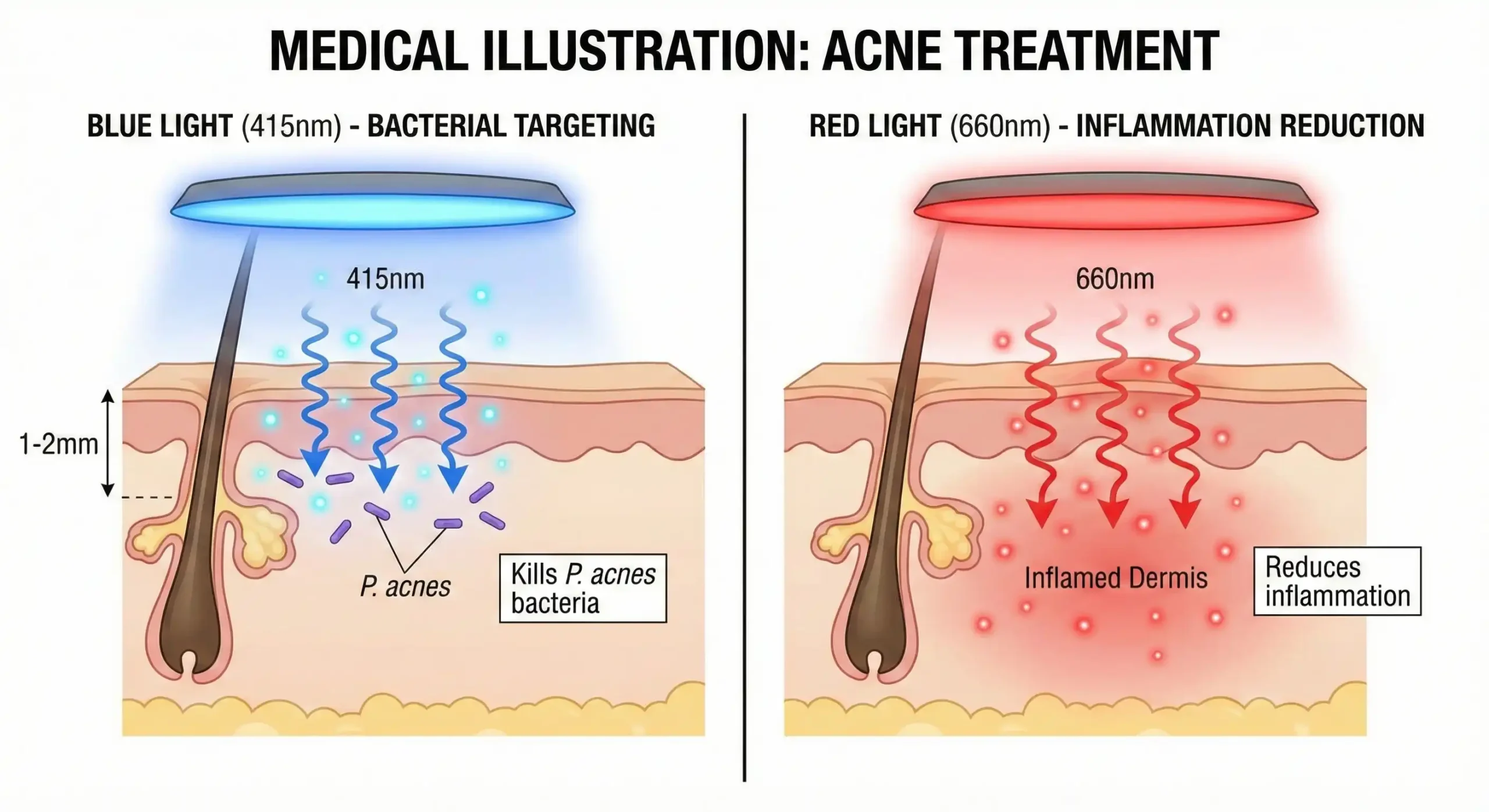
The mechanism difference: Red light (660nm) doesn’t kill P. acnes bacteria—that’s what blue light (415nm) does. Instead, red light reduces the inflammatory response that makes acne red, swollen, and painful. It also accelerates healing and reduces scarring. This is why the most effective acne protocols combine both wavelengths: blue light attacks bacteria, red light calms inflammation and speeds recovery. If you only use red light, you’re getting half the benefit.
Understanding Red Light Therapy in Practice
Red light therapy is often discussed in theory, but its real-world application depends on measurable parameters like wavelength and exposure. I tested multiple RLT setups using a professional spectrometer to better understand how the therapy works in practice.
Open Red Light HubHow Red Light Therapy Affects Acne (The Science)
Acne forms when three factors combine: excess sebum (oil) production, dead skin cells clogging pores, and bacterial overgrowth (primarily Propionibacterium acnes). The visible symptoms—redness, swelling, pain—are your immune system’s inflammatory response to these clogged, infected pores.
Red light therapy addresses acne through several mechanisms, but understanding what it does and doesn’t do is critical for realistic expectations.
What Red Light Actually Does for Acne
Anti-inflammatory action: When 660nm red light penetrates your skin (8-10mm depth), it’s absorbed by mitochondria in your cells, including immune cells surrounding inflamed acne lesions. This triggers a reduction in pro-inflammatory cytokines like IL-1β, IL-6, and TNF-α—the molecules that cause the redness, swelling, and pain in inflammatory acne. Clinical studies show red light can reduce inflammatory markers by 30-50% after 4-6 weeks of consistent use.
Accelerated wound healing: Red light stimulates fibroblasts to produce more collagen and increases cellular energy production (ATP). This means inflamed acne lesions heal faster, and the post-inflammatory hyperpigmentation (dark spots left after acne clears) fades more quickly. Studies show healing time can be reduced by 25-40% compared to no treatment.
Reduced sebum production: Some research suggests that near-infrared wavelengths (around 850nm) may help regulate sebaceous gland activity, reducing the excess oil production that contributes to acne formation. However, this effect is modest and not the primary mechanism.
Scar prevention: By reducing inflammation intensity and duration, red light minimizes the tissue damage that leads to acne scarring. It won’t reverse existing scars, but it can prevent new ones from forming as severe.
What Red Light Doesn’t Do for Acne
Does not kill bacteria: This is the most important distinction. Red light (660nm) does not have antibacterial properties against P. acnes. The wavelength that kills acne bacteria is blue light (415nm), which generates reactive oxygen species that are toxic to bacteria. If bacterial overgrowth is your primary issue, red light alone won’t be sufficient.
Limited effect on comedones: Blackheads and whiteheads (non-inflammatory acne) are primarily mechanical blockages—dead skin cells and sebum trapped in pores. Red light doesn’t unclog pores or exfoliate skin, so it has minimal direct effect on comedonal acne. You’ll need retinoids, salicylic acid, or other exfoliants for these.
Won’t fix hormonal root causes: If your acne is driven by hormonal imbalances (PCOS, high androgens, insulin resistance), red light manages symptoms but doesn’t address the root cause. Hormonal acne requires systemic treatment—diet, supplements, or medications.
Not effective for cystic acne alone: Deep, painful cystic acne involves inflammation below the reach of red light’s penetration depth. While red light may help somewhat, cystic acne typically requires prescription treatments (isotretinoin, hormonal therapy, corticosteroid injections).
The Research: Does Red Light Therapy Clear Acne?
The research on phototherapy for acne is extensive, though most studies focus on blue light or combination blue+red protocols rather than red light alone.
Red Light Studies
A 2007 study in The British Journal of Dermatology evaluated 660nm red light therapy in patients with mild-to-moderate acne. Treatment consisted of 15-minute sessions twice weekly for 4 weeks. Results:
- 34% reduction in inflammatory lesion count
- Significant improvement in patient-reported acne severity
- No adverse effects reported
- Benefits persisted for 8 weeks post-treatment
A 2009 study published in Lasers in Surgery and Medicine compared red light (660nm) alone versus blue light (415nm) alone versus combination therapy. Findings:
- Blue light alone: 46% reduction in inflammatory lesions
- Red light alone: 27% reduction in inflammatory lesions
- Combination blue+red: 76% reduction in inflammatory lesions
- Combination therapy was significantly superior to either wavelength alone
A 2014 meta-analysis in JAMA Dermatology reviewed 14 randomized controlled trials on light-based acne treatments. Conclusion: Red light monotherapy showed moderate efficacy for inflammatory acne, but combination therapy with blue light showed the strongest evidence of effectiveness.
Combination Therapy Evidence
The most compelling research supports using both blue and red light together:
Blue light (415nm):
- Penetrates 1-2mm into skin
- Activates porphyrins in P. acnes bacteria
- Generates reactive oxygen species that kill bacteria
- Primary effect: reduces bacterial load
Red light (660nm):
- Penetrates 8-10mm into skin
- Reduces inflammatory response
- Accelerates healing and collagen production
- Primary effect: calms inflammation, prevents scarring
When used sequentially (blue light first to kill bacteria, then red light to calm inflammation), the combined effect is synergistic—you’re attacking both the bacterial cause and the inflammatory symptoms.
Red Light Therapy Protocol for Acne
Based on the research and clinical use, here’s the evidence-based protocol:
| Parameter | Red Light Only | Combination (Blue + Red) |
|---|---|---|
| Wavelength | 660nm | 415nm (blue) + 660nm (red) |
| Distance | 6-8 inches from face | Same |
| Time per session | 10-15 minutes | 7-10 min blue, then 7-10 min red |
| Frequency | Daily (5-7x per week) | Daily (5-7x per week) |
| Duration | Minimum 4-6 weeks | Minimum 4-6 weeks |
| Target dose | 10-20 J/cm² per session | 10-15 J/cm² each wavelength |
| Best for | Inflammatory acne, healing, scar prevention | Moderate-severe acne, bacterial component |
Step-by-Step Treatment Process
1. Cleanse thoroughly: Remove all makeup, sunscreen, and oil from your face. Use a gentle cleanser. Pat dry completely. Any residue on your skin can interfere with light penetration or cause irritation when activated by light.
2. Position yourself: Sit or stand 6-8 inches from your red light device. Most facial devices are handheld or have a stand for hands-free use. The light should cover your entire face or the affected area.
3. Protect your eyes: Close your eyes during treatment. Most red light isn’t bright enough to cause damage, but prolonged direct exposure can be uncomfortable. Some devices come with protective goggles—use them if provided.
4. Start treatment:
- Red light only: 10-15 minutes, face relaxed
- Combination protocol:
- 7-10 minutes blue light first (kills bacteria)
- Immediate follow-up: 7-10 minutes red light (reduces inflammation)
5. Post-treatment: You can immediately apply your normal skincare products. In fact, some evidence suggests red light may enhance absorption of topicals applied immediately after treatment.
6. Consistency is critical: Unlike taking a pill, red light therapy requires daily consistency for 4-8 weeks to see significant results. Missing 2-3 days per week significantly reduces effectiveness.
Timing Strategies
Morning treatment: Many people prefer morning sessions. Clean face after waking, do red light therapy, then apply morning skincare routine (moisturizer, sunscreen). This fits easily into existing routines.
Evening treatment: Equally effective. Some prefer evening because you’re not rushing to get out the door. Clean face after removing makeup, do therapy, then apply nighttime products (retinoids, moisturizers).
Avoid immediately after strong actives: If you use potent retinoids, AHAs, or BHAs, wait 20-30 minutes after applying them before doing red light therapy to avoid potential irritation from increased absorption.
Realistic Timeline: When to Expect Results
Red light therapy for acne is not an overnight solution. Here’s what to expect:
Week 1-2: Minimal visible change
- You might notice slightly reduced redness by end of week 2
- Some people report less morning puffiness/inflammation
- New breakouts may still appear (existing clogs working their way out)
- Don’t get discouraged—cellular changes are happening even if not visible yet
Week 3-4: Subtle improvements
- Existing inflammatory lesions heal 20-30% faster than usual
- New breakouts may be less severe (smaller, less red)
- Post-inflammatory marks (dark spots) begin fading slightly
- Skin tone may look more even
Week 5-8: Clear benefits
- Inflammatory lesion count reduces by 30-50%
- Breakouts are less frequent and less severe
- Healing time significantly improved
- Post-inflammatory hyperpigmentation noticeably lighter
- Skin texture smoother
Week 9-12: Continued improvement
- Approaching maximum benefit for current protocol
- Maintenance phase—continue treatment to sustain results
- May be able to reduce frequency to 3-5x per week
After stopping: Benefits gradually diminish over 2-4 weeks. Acne will return to baseline unless you continue treatment or address root causes (hormones, diet, skincare).
What Success Looks Like
Best-case scenario (inflammatory acne, consistent use, combination therapy):
- 60-80% reduction in inflammatory lesions
- Faster healing (5-7 days instead of 10-14 days)
- Minimal new scarring
- More even skin tone
Typical scenario (red light only, moderate consistency):
- 30-50% reduction in inflammatory lesions
- Moderately faster healing
- Some improvement in hyperpigmentation
- Continued breakouts but less severe
Poor response (wrong acne type or poor consistency):
- <20% improvement
- Still frequent breakouts
- Minimal change in healing time
Combining Red Light With Other Acne Treatments
Red light therapy works best as part of a comprehensive acne treatment strategy, not as a standalone solution.
Synergistic Combinations
Red Light + Blue Light: As discussed, this is the gold standard. Blue light kills bacteria, red light calms inflammation. Many devices now offer both wavelengths in one unit.
Red Light + Retinoids (tretinoin, adapalene): Excellent combination. Retinoids unclog pores and increase cell turnover (preventing new acne), while red light reduces the inflammation and accelerates healing. Apply retinoid in the evening, do red light therapy in the morning, or vice versa with a 30-minute gap.
Red Light + Salicylic Acid: Salicylic acid (BHA) exfoliates inside pores, removing dead skin cells and oil. Red light handles inflammation and healing. Use salicylic acid cleanser or toner, then do red light therapy after skin is dry.
Red Light + Niacinamide: Niacinamide regulates sebum production and has its own anti-inflammatory properties. Apply niacinamide serum, let it absorb for 5-10 minutes, then do red light therapy. They work synergistically.
Red Light + Oral Supplements: Zinc, omega-3s, and probiotics address acne from the inside. Red light addresses external inflammation. Combining systemic and topical approaches often yields best results.
What Not to Combine
Avoid: Red Light + Photosensitizing medications: Some antibiotics (tetracyclines), retinoids (isotretinoin), and other medications increase photosensitivity. Consult your dermatologist if you’re on any prescription acne treatments before starting light therapy.
Avoid: Red Light immediately after chemical peels or laser treatments: Wait 1-2 weeks after any aggressive professional treatments. Your skin barrier needs to recover first.
Be cautious: Red Light + high-percentage AHAs: Glycolic acid, lactic acid peels, and other strong exfoliants may make skin more sensitive. If using these, do red light therapy on alternate days or wait several hours after application.
Device Selection for Acne Treatment
Not all red light devices are appropriate for facial acne treatment. Here’s what to look for:
Key Specifications
Wavelength requirements:
- Essential: 660nm (red) for inflammation
- Ideal: 660nm + 415nm (blue) for comprehensive treatment
- Avoid: Devices that only offer 850nm (near-infrared) without 660nm—these don’t address acne effectively
Power output:
- Minimum: 30-50 mW/cm² at treatment distance
- Ideal: 60-100 mW/cm² for shorter treatment times
- Measure at 6-8 inches (typical facial treatment distance)
Coverage area:
- Face-specific devices: 6×8 inches or larger
- Handheld spot-treatment: 3×5 inches (for targeted areas only)
- Full face coverage is more efficient than spot-treating
Safety features:
- Eye protection (built-in or goggles provided)
- Timer function (prevents overexposure)
- Low EMF emission
- FDA clearance (if making medical claims)
Stop Guessing Your Session Time
10 minutes on a weak panel is nothing. 10 minutes on a pro panel is an overdose. Calculate your exact personalized dose.
Device Categories
LED face masks ($100-300):
- Pros: Hands-free, cover entire face, easy to use
- Cons: Some only offer blue light, not combination; variable quality
- Best for: Consistent daily users who want convenience
Handheld panels ($150-400):
- Pros: Targeted treatment, portable, often combination blue+red
- Cons: Requires holding for 10-15 minutes
- Best for: Spot-treating specific areas or alternating face zones
Large panels ($300-800):
- Pros: Treat face and other body acne (chest, back), multi-purpose
- Cons: Bulky, overkill if only treating face
- Best for: People with body acne or who want full-body benefits too
Professional devices ($1000+):
- Pros: Higher power, clinical-grade, faster results
- Cons: Expensive, overkill for home use
- Best for: Severe acne, professional treatment rooms
Who Should (and Shouldn’t) Try Red Light for Acne
Good Candidates
Inflammatory acne sufferers: If your acne is primarily red, swollen papules and pustules (not deep cysts or just blackheads), red light will help significantly.
People who can’t tolerate harsh topicals: If retinoids, benzoyl peroxide, or acids irritate your skin too much, red light provides an anti-inflammatory alternative without chemical irritation.
Post-acne hyperpigmentation: If you have dark spots from past breakouts, red light accelerates fading of these marks.
Mild-to-moderate acne: Best response rate. Severe cystic acne typically needs more aggressive treatment, but red light can be adjunctive.
Maintenance after Accutane: Many people use red light therapy to maintain clear skin after completing isotretinoin treatment.
Poor Candidates or Need Modifications
Cystic acne as primary concern: Deep cysts are below red light’s penetration depth. You’ll need prescription treatments. Red light can be supplementary but won’t solve cystic acne alone.
Comedonal acne only: If you primarily have blackheads and whiteheads with minimal inflammation, red light won’t do much. You need pore-clearing actives (retinoids, salicylic acid).
Hormonal acne without addressing root cause: PCOS, high androgens, insulin resistance—these need systemic treatment. Red light manages symptoms but won’t fix hormones.
People on photosensitizing medications: Check with your doctor first. Some medications increase risk of adverse reactions to light therapy.
Very dark skin tones: Red light still works, but you may need slightly longer treatment times or higher power output because melanin absorbs some of the light. Studies show efficacy across all skin types, just with dose adjustments.
Common Questions About Red Light Therapy for Acne
Can red light therapy make acne worse initially?
Yes, a small percentage of people experience a “purging” phase in weeks 2-4 where acne temporarily worsens before improving. This happens because red light may stimulate cellular turnover and sebum gland activity, bringing existing clogs to the surface faster. If purging occurs, it typically resolves by week 4-5. However, if new severe breakouts appear that weren’t there before, discontinue and consult a dermatologist—this could be an adverse reaction rather than purging.
How does red light compare to prescription acne treatments?
They’re complementary, not competitive. Prescription treatments (isotretinoin, spironolactone, topical retinoids) address root causes—hormones, pore structure, sebum production. They’re more powerful for moderate-severe acne. Red light therapy manages inflammation and healing but doesn’t fix underlying causes. Most dermatologists view red light as a good adjunctive therapy that can reduce the need for harsh topicals or antibiotics, but not a replacement for prescriptions in moderate-severe cases.
Do I need to keep using red light therapy forever, or will acne stay gone?
Unfortunately, acne usually returns when you stop red light therapy if underlying causes haven’t been addressed. Think of it like using a retinoid—it works while you use it, but if you stop, acne comes back. To maintain results, most people either: (1) continue red light 2-3x per week as maintenance, or (2) pair it with long-term solutions like diet changes, hormonal management, or retinoid use.
Can I use red light therapy while pregnant or breastfeeding?
Red light therapy is generally considered safe during pregnancy and breastfeeding—it’s non-invasive, doesn’t use chemicals, and doesn’t penetrate deep enough to affect a fetus. However, research specifically in pregnant women is limited. Many pregnant women develop acne due to hormonal changes and appreciate having a non-medication option. That said, always consult your OB-GYN before starting any new treatment during pregnancy, including red light therapy.
INTERNAL LINKS
For comprehensive acne management beyond red light therapy:
- Understand device specifications in red light therapy ultimate guide
- Learn proper dosing in red light therapy dosing guide
- See wavelength differences in 660nm vs 850nm comparison
- Get complete setup instructions in how to use red light therapy at home
- Check realistic timelines in how long does red light therapy take to work
SOURCES
- Red light therapy for acne vulgaris: Papageorgiou, P., et al. “Phototherapy with blue (415 nm) and red (660 nm) light in the treatment of acne vulgaris.” British Journal of Dermatology, 2000. https://pubmed.ncbi.nlm.nih.gov/10671773/
- Combination blue and red light therapy: Gold, M.H., et al. “Clinical efficacy of self-applied blue light therapy for mild-to-moderate facial acne.” Journal of Clinical and Aesthetic Dermatology, 2009. https://pubmed.ncbi.nlm.nih.gov/20725545/
- Mechanisms of phototherapy in acne: Barolet, D., et al. “Infrared and skin: Friend or foe.” Journal of Photochemistry and Photobiology B: Biology, 2016. https://pubmed.ncbi.nlm.nih.gov/26745730/
- Meta-analysis of light-based acne treatments: Hamilton, F.L., et al. “Laser and other light therapies for the treatment of acne vulgaris: systematic review.” British Journal of Dermatology, 2009. https://pubmed.ncbi.nlm.nih.gov/19298294/
- Anti-inflammatory effects of red light: Avci, P., et al. “Low-level laser (light) therapy (LLLT) in skin: stimulating, healing, restoring.” Seminars in Cutaneous Medicine and Surgery, 2013. https://pubmed.ncbi.nlm.nih.gov/24049929/
